Don’t ignore new floaters.
Floaters are grossly defined as anything which moves back and forth in your vision as your eye moves: up and down or side to side. While floaters are very common, they are not necessarily benign.
Floaters can be the first sign that you have a retinal tear or retinal detachment.
What are Floaters?
Floaters are in the vitreous. The vitreous is the watery gel which fills your eye. As your eye moves, the gel swishes back and forth inside the eye.
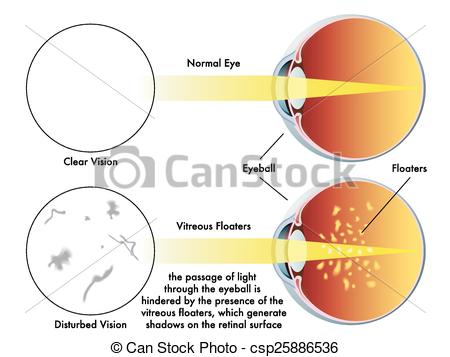
Blood, retinal tissue, inflammatory cells or a change in the clarity of the eye can cast shadows on your retina causing dark spots moving in your vision. These are generically called “floaters.”
Blood, called a vitreous hemorrhage, can occur from a retinal tear or in certain cases of diabetic retinopathy. Certain retinal vascular diseases can cause a vitreous hemorrhage as well.
Cells normally found underneath the retina can migrate to the vitreous through a retinal tear. These cells are large enough or clump together to cause visible floaters.
Inflammatory cells can also migrate to the vitreous in certain types of inflammation caused by either infection or non-infectious causes (e.g. auto-immune).
New Floaters
New onset of floaters need to be examined. It’s impossible to tell the cause of the floaters, but the fear is that the floaters are due to a retinal tear. Retinal tears can cause retinal detachments which require surgery and possible loss of vision.
Retinal tears, if identified before are retinal detachment has occurred, can be treated with laser instead of intraocular surgery.
The only way to be positive new floaters are NOT due to a retinal tear is by examining your retina by dilating your pupils.
Even if you have had long standing floaters, but suddenly get an increase in floaters, we recommend you alert your eye doctor.